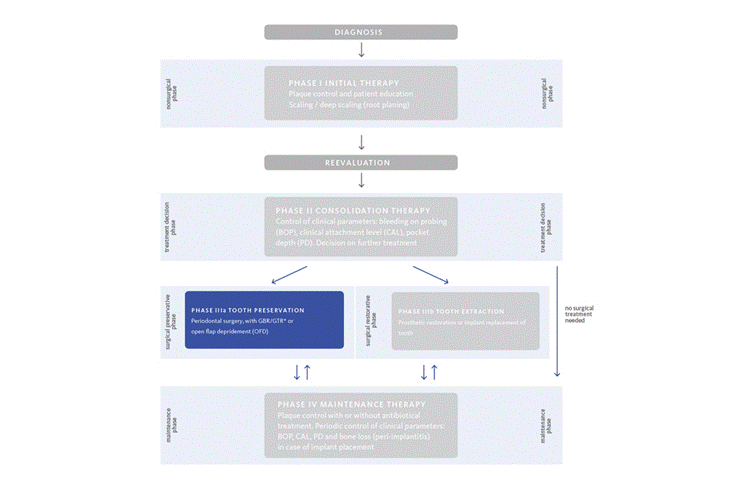
Periodontal - Diagnosis
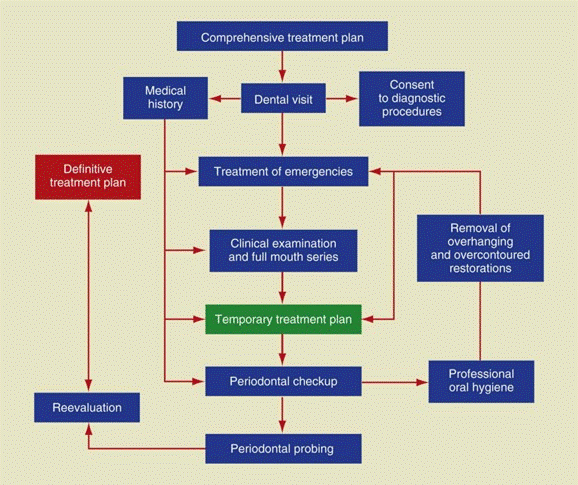

Clinical Examination
- Bleeding gums during brushing or eating
- Increasing spacing between their teeth
- Usually painless, but sometimes localized dull pain radiating deep into the jaw
- Sensitivity due to exposed roots
- Halitosis
- Gingival tenderness and itchiness
- Loose teeth

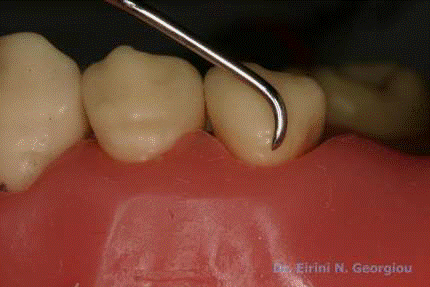
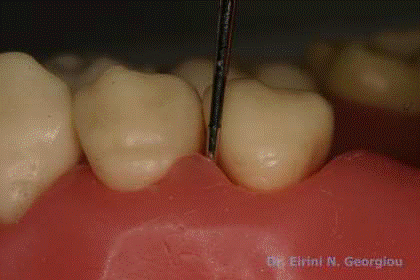
Visible light
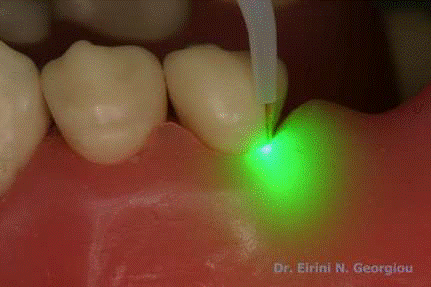
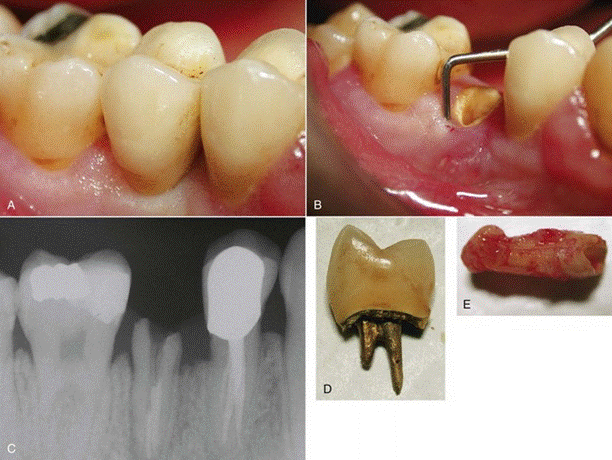

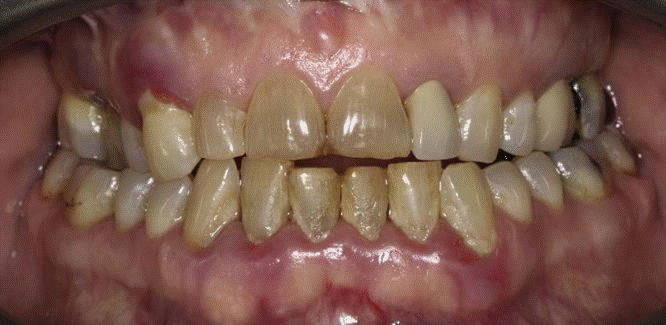
Probing the Pocket depth Vs attachment level
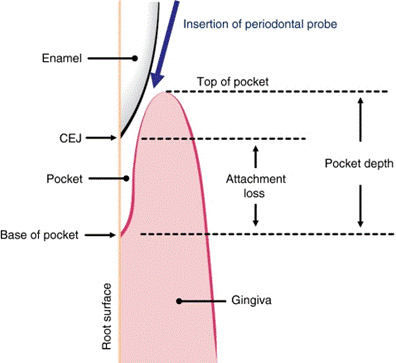

Top left, Detection of the smoothness of various irregularities on the root surface with the outward motion of a probe or explorer. Top center, Calculus. Top right, Caries. Bottom left and right, Irregular margins of restorations.
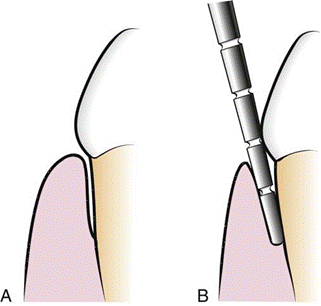
The biologic or histologic pocket depth is the actual distance between the gingival margin and the attached tissues (i.e., the bottom of the pocket). B, The probing or clinical pocket depth is the depth of penetration of the probe.
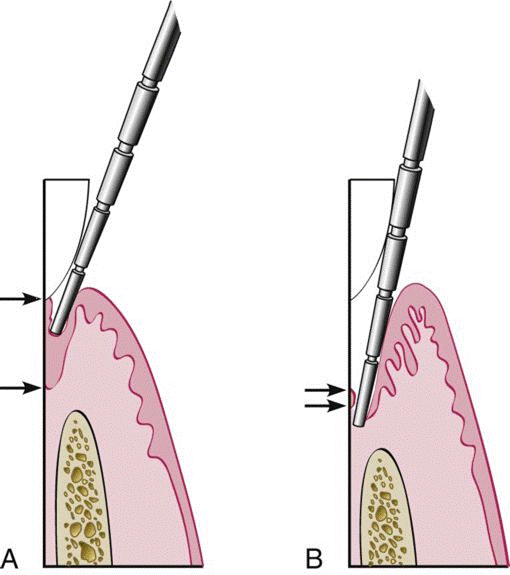
In a normal sulcus with a long junctional epithelium (between arrows), the probe penetrates about one third to half the length of the junctional epithelium. B, In a periodontal pocket with a short junctional epithelium (between arrows), the probe penetrates beyond the apical end of the junctional epithelium.

“Walking” the probe to explore the entire pocket
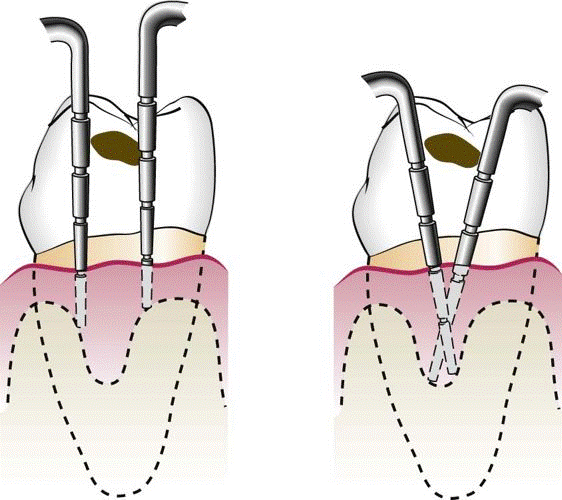
Vertical insertion of the probe (left) may not detect interdental craters; oblique positioning of the probe (right) reaches the depth of the crater.
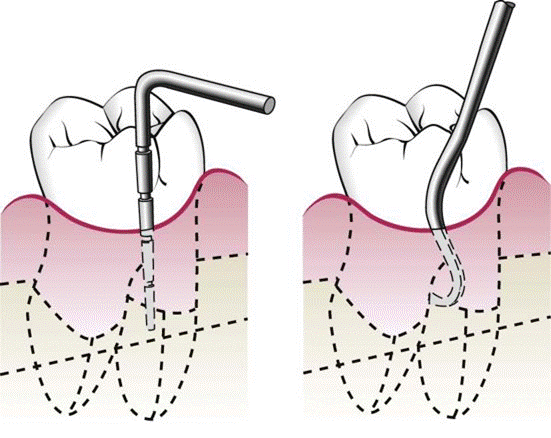
Exploring with a periodontal probe (left) may not detect furcation involvement; specially designed instruments (i.e., Nabers probes) (right) can enter the furcation area.

The limitations of periodontal probing. B, Probing pressure caused by probe angulation, the presence of subgingival calculus, and the presence of overhanging restorations.

Automated periodontal probes: Florida Probe System. Integration of direct electronic measurements with constant probing force, with computer storage and online data readout
Palpation
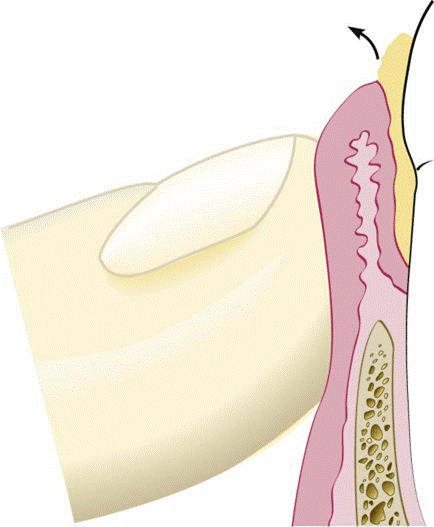
Palpation: Purulent exudate expressed from a periodontal pocket by digital pressure.
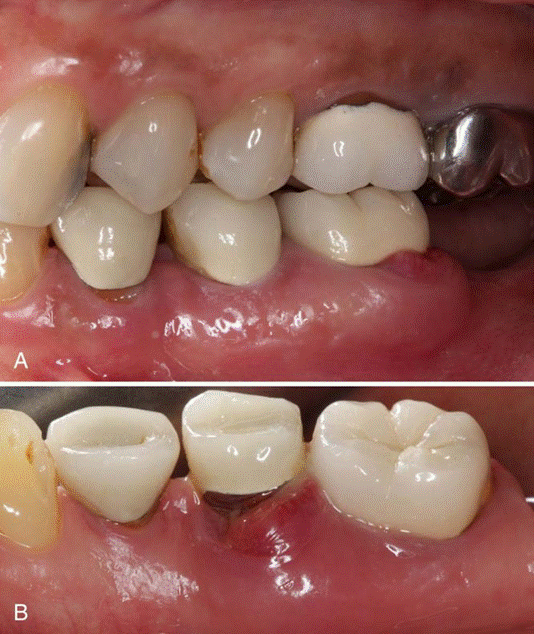
Acute periodontal abscesses on A, the buccal aspect of tooth #36 and B, the lingual aspect of tooth #35 in the same patient.
Periodontal charting
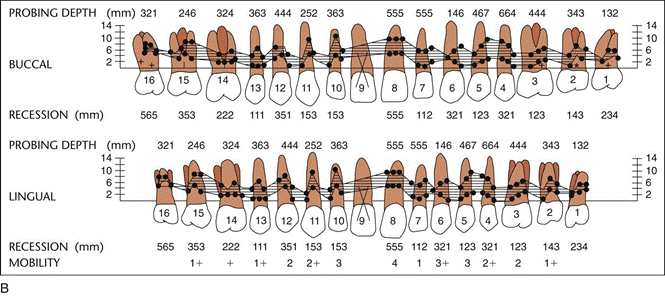
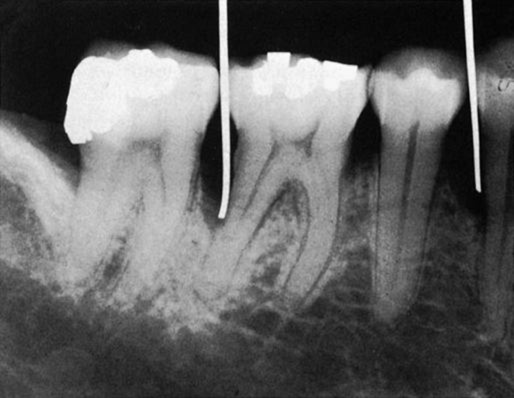
Radiographic Aids in the Diagnosis of Periodontal Disease
Normal Interdental Bone
Evaluation of bone changes in periodontal disease is based mainly on the appearance of the interdental bone because the relatively dense root structure obscures the facial and lingual bony plates. The interdental bone normally is outlined by a thin, radiopaque line adjacent to the periodontal ligament (PDL) and at the alveolar crest, referred to as the lamina dura. Because the lamina dura represents the cortical bone lining the tooth socket, the shape and position of the root and changes in the angulation of the x-ray beam produce considerable variations in its appearance.
The width and shape of the interdental bone and the angle of the crest normally vary according to the convexity of the proximal tooth surfaces and the level of the cementoenamel junction (CEJ) of the approximating teeth. The faciolingual diameter of the bone is related to the width of the proximal root surface. The angulation of the crest of the interdental septum is generally parallel to a line between the CEJs of the approximating teeth.When there is a difference in the level of the CEJs, the crest of the interdental bone appears angulated rather than horizontal.
Prichard established the following four criteria to determine adequate angulation of periapical radiographs:
- The radiograph should show the tips of molar cusps with little or none of the occlusal surface showing.
- Enamel caps and pulp chambers should be distinct.
- Interproximal spaces should be open.
- Proximal contacts should not overlap unless teeth are out of line anatomically.
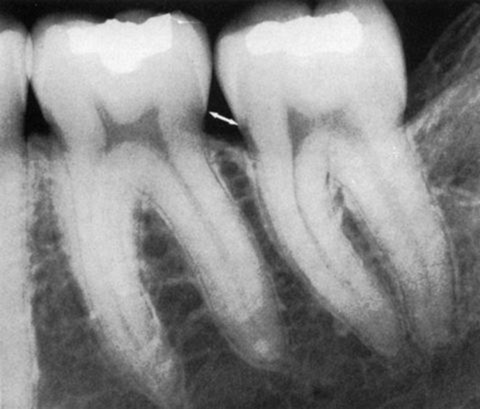
Crest of interdental bone normally parallel to a line drawn between the cementoenamel junction of adjacent teeth (arrow). Note also the radiopaque lamina dura around the roots and interdental bone.
Bone Destruction in Periodontal Disease
The slight radiographic changes of the periodontal tissues suggest that the disease has progressed beyond its earliest stage
- Bone Loss:The difference between the alveolar crest height and the radiographic appearance ranges from 0 to 1.6 mm, mostly accounted for by x-ray angulation.
- Amount: The amount of bone loss is estimated to be the difference between the physiologic bone level and the height of the remaining bone.
The distance from the CEJ to the alveolar crest has been suggested to be a distance of 2 mm to reflect normal periodontium; this distance may be greater in older patients.
- Distribution: The distribution of bone loss is an important diagnostic sign. It points to the location of destructive local factors
- Pattern of Bone Destruction:In Periodontal disease
The interdental bone undergoes changes that affect the lamina dura, crestal radiodensity, size and shape of the medullary spaces, and height and contour of the bone. Height of interdental bone may be reduced, with the crest perpendicular to the long axis of the adjacent teeth (horizontal bone loss), or angular or arcuate defects (angular, or vertical, bone loss) could form.
Dense cortical facial and lingual plates of interdental bone obscure destruction of the intervening cancellous bone. Thus a deep craterlike defect between the facial and lingual plates might not be depicted on conventional radiographs. To record destruction of the interproximal cancellous bone radiographically, the cortical bone must be involved. A reduction of only 0.5 to 1.0 mm in the thickness of the cortical plate is sufficient to permit radiographic visualization of the destruction of the inner cancellous trabeculae
Radiographic Appearance of Periodontal Disease

Fuzziness and disruption of lamina dura crestal cortication continuity is the earliest radiographic change in periodontitis and results from bone resorption activated by extension of gingival inflammation into the periodontal bone.
Continued periodontal bone loss and widening of the periodontal space results in a wedge-shaped radiolucency at the mesial or distal aspect of the crest

Generalized horizontal bone loss.
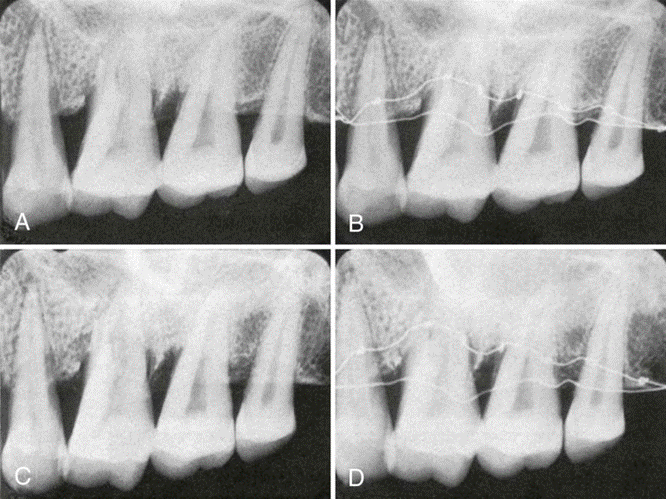
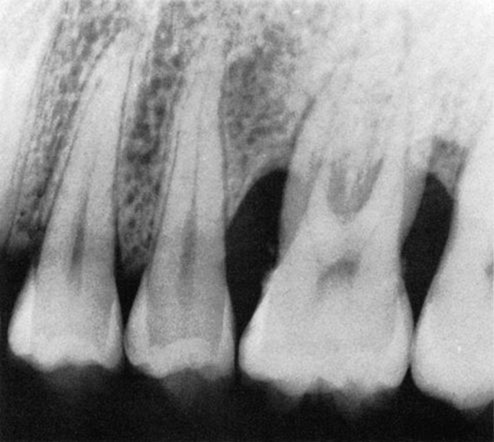
Angular bone loss on first molar with involvement of the furcation.
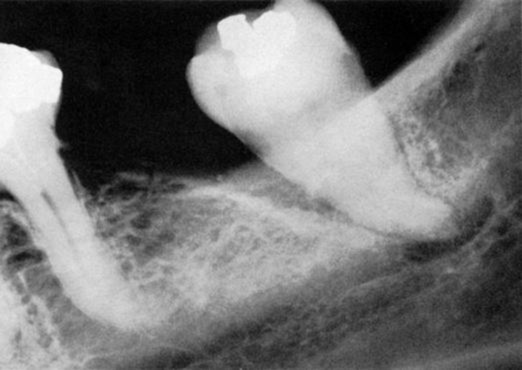
Angular bone loss on a mandibular molar partially obscured by a dense mylohyoid ridge.
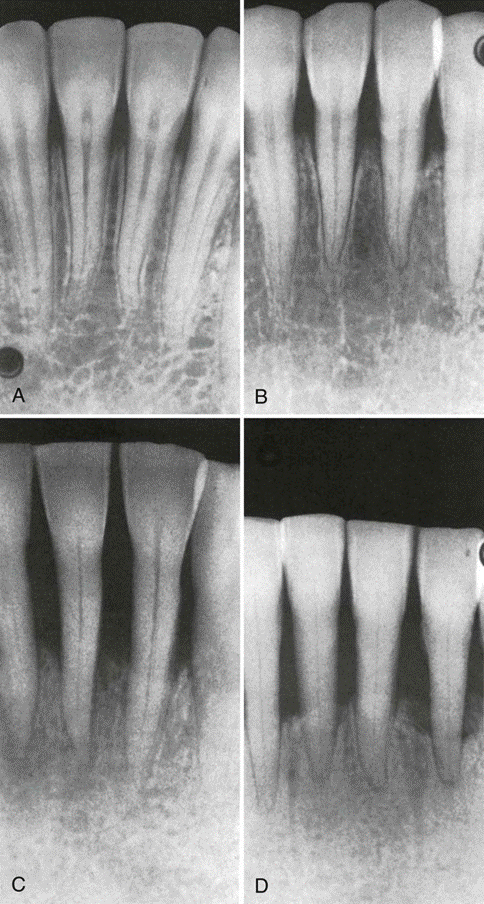
Furcation Involvement
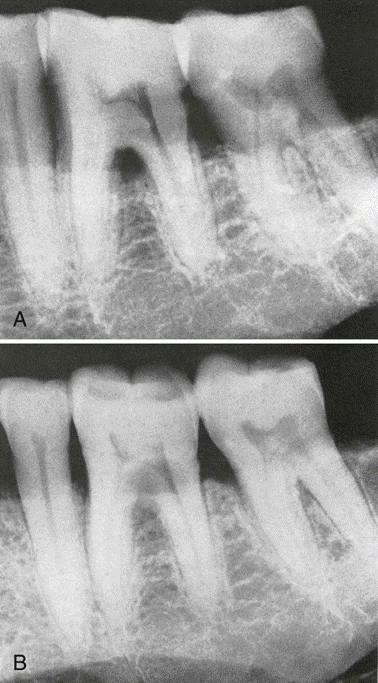
Furcation Involvement indicated by triangular radiolucency in the bifurcation area of mandibular first molar.

Furcation involvement of mandibular first and second molars indicated by thickening of periodontal space in the furcation area. The furcation of the third molar is also involved, but the thickening of the periodontal space is partially obscured by the external oblique line.
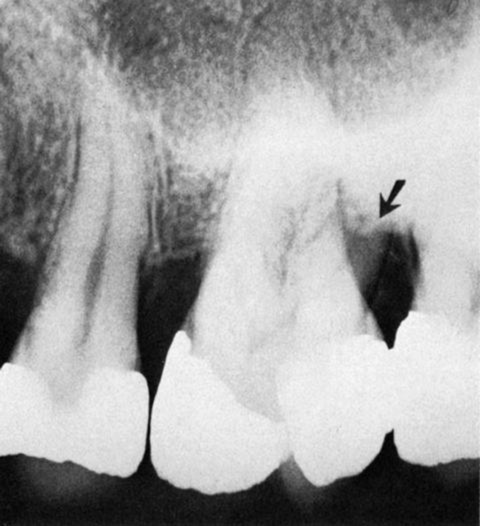
Furcation involvement of the first molar partially obscured by the radiopaque lingual root. The horizontal line across the distobuccal root demarcates the apical portion (arrow), which is covered by bone, from the remainder of the root, where the bone has been destroyed.
Periodontal abscess: Localised aggressive bone loss
Radiolucent area on lateral aspect of root with periodontal abscess.
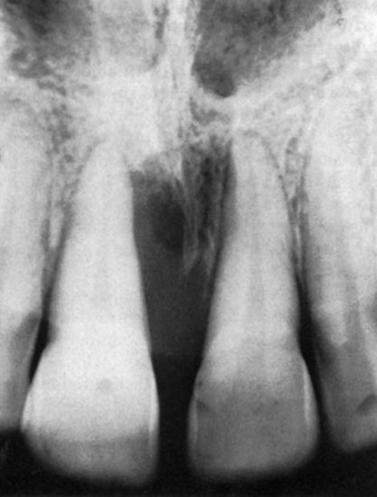
Radiographic appearance of periodontal abscess on right central incisor.
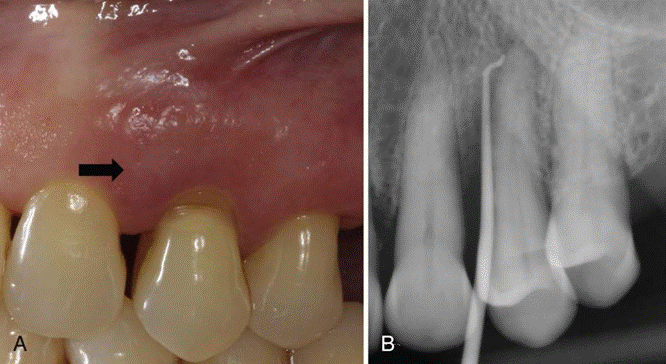
Periodontal abscess. A, Periodontal abscess in the left maxillary first premolar area. B, Extensive bone destruction on the mesial surface of the first premolar. Gutta-percha point traces to the root apex.
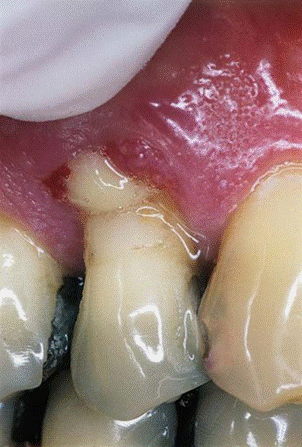
Gentle digital pressure may be sufficient to express purulent discharge.
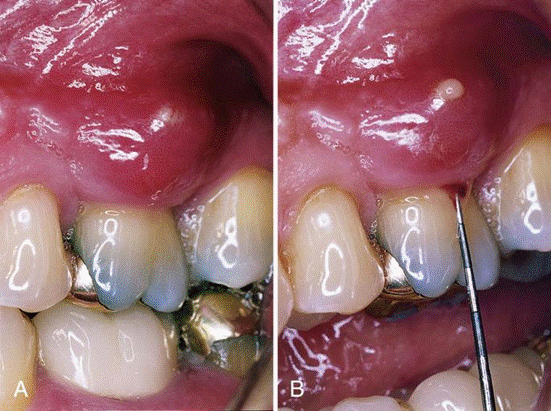
Periodontal abscess of maxillary left first molar. B, Periodontal probe is used to gently retract the pocket wall.
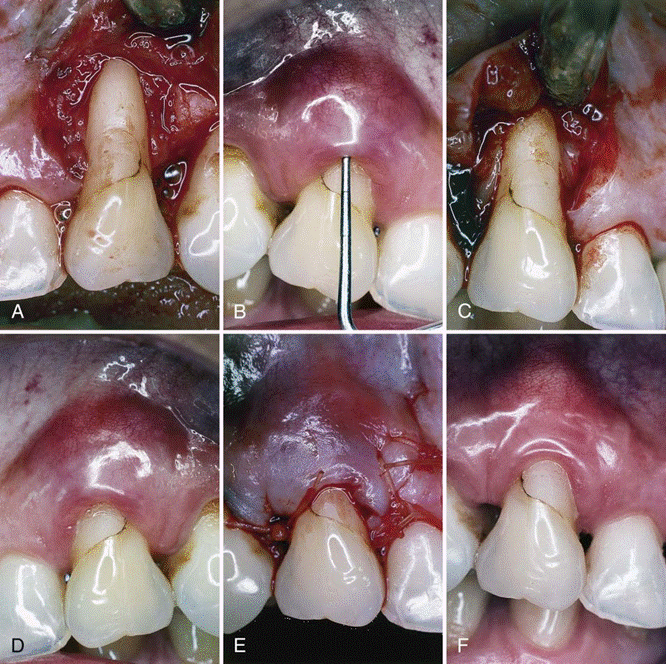
Periodontal abscess of maxillary right canine. B, Using local anesthesia, periodontal probe is inserted to determine severity of the lesion. C, Using mesial and distal vertical incisions, a full-thickness flap is elevated, exposing severe bone dehiscence, a subgingival restoration, and root calculus. D, Root surface has been planed free of calculus and the restoration smoothed. E, Full-thickness flap has been replaced to its original position and sutured with absorbable sutures. F, At 3 months, gingival tissues are pink, firm, and well adapted to the tooth, with minimal periodontal probing depth.